In brief
- Quincke’s edema = rapid swelling of the face, neck, or throat that can lead to airway obstruction.
- Mainly related to an allergic reaction: foods (eggs, seafood, peanuts), medications, insect stings.
- Recognizing symptoms early (hoarse voice, difficulty swallowing, hives) increases the chances of rapid and effective management.
- In case of suspected anaphylaxis, call emergency medical services and administer adrenaline if available.
- Prevention relies on avoidance diet, family education, and follow-up with an allergist for a personalized action plan.
Quickly recognize the symptoms of Quincke’s edema in children
Parents sometimes see a simple redness evolve into a more worrying condition. It is essential to learn to spot the early signs of Quincke’s edema or angioedema in children. These signs make it possible to act quickly, as progression can be very rapid.
The first common sign is a sudden swelling of the face, eyelids, lips, or neck region. The voice may become more hoarse and repetitive throat clearing sounds may be heard. Sometimes, the child complains of a tickling sensation in the throat, then difficulty swallowing.
Before visible swelling appears, other manifestations can warn: a generalized skin rash (hives), itching on the chest or limbs, nasal discharge, or dry cough. Digestive symptoms such as intense abdominal pain, nausea, or vomiting may precede or accompany the reaction.
A concrete example: at a birthday party, Lucas, 6 years old, tasted an apparently harmless cake. Fifteen minutes later, he had itching and his voice changed. The parents noticed swelling around the lips. Their quick reaction prevented worsening. This kind of anecdote shows that an allergic reaction can occur at the first obvious ingestion or upon re-exposure.
It is also important to know the signs of severity. Wheezing, cyanosis (bluish lips), or clear respiratory distress require immediate alerting of emergency medical services. The earlier anaphylaxis begins after exposure, the more severe it can be: a reaction occurring within minutes poses a higher risk than a delayed reaction.
To visually sort out: localized swelling around the eyes or lips is not always synonymous with airway obstruction, but laryngeal swelling (perceived by hoarse voice, barking cough) is an emergency. Parents should consider all signs: skin, respiratory, digestive, and behavioral (agitation, drowsiness).
A final practical tip: having a simple notebook with allergy history, the date and suspected food, and treatments already tried facilitates communication with emergency services. This organization reduces anxiety and allows for smoother management. Insight: early detection of several associated symptoms significantly increases the child’s safety.
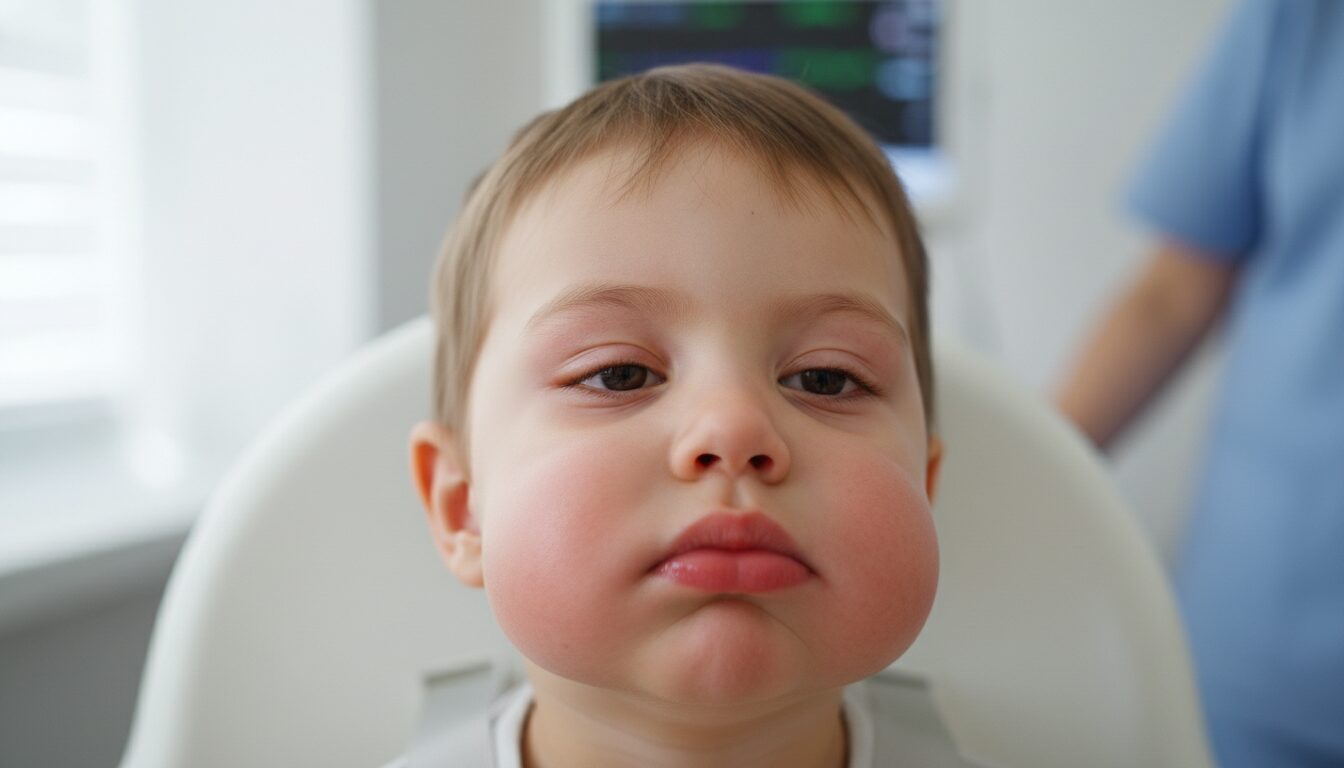
Causes and mechanisms of angioedema: why does Quincke’s edema occur?
Understanding the mechanism behind Quincke’s edema helps better anticipate risky situations. The key is that the body releases inflammatory mediators, mainly histamine, in response to a stimulus perceived as dangerous.
During an immediate-type allergic reaction (IgE-mediated), exposure to the allergen triggers degranulation of mast cells and basophils. This releases histamine which increases vascular permeability, causing localized swelling of tissues. If structures of the larynx are affected, the child may present threatening angioedema.
There are also non-allergic oedemas, rarer, related to other mediators such as leukotrienes or bradykinin. For example, certain medications (aspirin, angiotensin-converting enzyme inhibitors) can trigger bradykinin-mediated edema. These forms do not always involve elevated IgE and may require a different approach to prevention.
A common case in pediatrics is food allergy. Foods often involved are eggs, milk, peanuts, seafood, and tree nuts. In children with a history of eczema or hives, the probability of a more severe reaction upon repeated exposure is increased.
Illustration: Sophie, mother of a 2-year-old girl, observed that the child’s initial reactions were limited to eczema after ingesting a food. At the second exposure, the child developed breathing difficulties and cervical swelling. The clinical history shows that manifestations often evolve: early skin symptoms may precede a more severe manifestation.
Timing matters: edema appearing within minutes requires extreme vigilance. Biologically, the inflammatory cascade can lead to anaphylactic shock if vasodilation and plasma leakage are massive, causing hypotension and circulatory disorders.
For professionals and parents, distinguishing an allergic edema from a drug-induced edema or one linked to a genetic pathology (hereditary edema) is crucial. The allergist plays a central role in the investigation: skin tests, blood tests, and discussions about risks. Insight: understanding the mediator involved guides prevention and treatment choices.
What to do in a medical emergency: actions to take immediately in case of Quincke’s edema
Faced with a suspected reaction, the priority is to secure breathing and quickly call emergency services. Medical emergency must be contacted as soon as respiratory signs appear or if the child shows distress symptoms.
Concrete steps and their order: first, position the child sitting or semi-sitting to facilitate ventilation. Avoid laying the child flat if breathing is compromised. Then, if the child has a prescribed adrenaline auto-injector (epipen), it must be administered immediately according to medical recommendations.
Here is a practical list every parent should know:
- Call the emergency number (in France 15 or 112 depending on the situation).
- Administer intramuscular adrenaline if available and prescribed.
- Place the child in a sitting position and ensure maximum ventilation of the room.
- Do not leave the child alone and note the time of adrenaline administration.
- Inform emergency services of allergy history and medications given.
An example: the Martin family, faced with a rash followed by coughing and changed voice, used the auto-injector for their 7-year-old son and immediately called emergency services. The rapid intervention allowed hospital management without intubation.
At the hospital, the medical team can complete treatment with oxygen, antihistamines, corticosteroids, and, if necessary, a second injection of adrenaline. In case of severe obstruction, intubation or emergency tracheotomy procedures may be considered by the anesthesia team. The decision depends on clinical status and speed of progression.
Important to remember: adrenaline is not contraindicated even if the diagnosis is uncertain and the situation seems serious. Waiting can be more dangerous than administering the treatment. Vigilance must remain high for the following hours due to the risk of biphasic reaction.
Finally, upon returning home, organizing follow-up with an allergist and updating the written action plan is essential. Insight: first aid and intramuscular adrenaline save lives; preparation and speed make all the difference.
Treatments, allergological follow-up, and prevention of recurrences
After initial management of Quincke’s edema, structured medical follow-up is key to reducing future risks. Allergological consultation helps identify the causative allergen and establish an adapted prevention plan for the child.
Hospital treatment often includes corticosteroids to reduce inflammation, antihistamines to control skin symptoms, and prolonged monitoring to detect any secondary reaction. If airway obstruction threatened breathing, an intervention (intubation, tracheotomy) may have been performed and ICU follow-up required.
Upon discharge, prescribing an adrenaline auto-injector is systematically considered when the risk of anaphylaxis is documented. Education of parents and close contacts on how to use this auto-injector is essential. Schools and childcare facilities must also be informed and trained if necessary.
Here is a useful summary table for parents and caregivers:
| Common allergen | Usual onset time | Recommended action |
|---|---|---|
| Peanuts, tree nuts | Minutes to 2 hours | Total avoidance, auto-injector prescribed if history |
| Eggs, milk | Minutes to 2 hours | Allergological follow-up; controlled reintroduction based on tests |
| Medications (aspirin, beta blockers) | Immediate to delayed | Avoidance, therapeutic alternative, alert documentation |
| Insect stings (wasp, hornet) | Minutes | Avoidance, emergency treatment, possible desensitization |
Prevention involves a clearly explained avoidance diet adapted to daily life. For a child at school, a written protocol, a label on the medical file, and supporting documents simplify management. Early and supervised food diversification, validated by the doctor, can reduce some long-term food allergy risks according to current recommendations.
Specific therapies, such as oral immunotherapy for peanut allergy, have emerged in recent years and should be discussed with an allergist. They are not systematic but can be proposed in specialized centers to reduce sensitivity to the allergen.
Finally, to support families and reduce guilt, practical and caring resources exist. The platform La Vie de Bébé offers concrete benchmarks for daily life and parental support. Insight: structured care after the acute episode allows turning a potentially traumatic situation into a safe and controlled path for the family.
How to differentiate a benign swelling from a potentially serious Quincke’s edema?
Localized swelling without respiratory signs is often less urgent. However, the presence of hoarse voice, difficulty swallowing, wheezing, or general malaise requires immediate alerting of emergency services.
My child has an adrenaline auto-injector: how to ensure it is correctly used?
Practical sessions with a healthcare professional, regular demonstrations, and repetitions using a training device are recommended. Note the expiration date and replace the auto-injector as needed.
Can Quincke’s edema be prevented by modifying the infant’s diet?
Food diversification guided by the pediatrician or allergist, without unjustified early elimination, is recommended. Some recent studies show that controlled introduction may reduce allergy risk for certain foods.
What to do if the responsible allergen is unknown?
Consult an allergist for appropriate tests (prick tests, specific IgE) and establish an action plan. Meanwhile, avoid suspected foods and inform the child’s care structures.