In brief :
- Pilonidal cyst: small benign nodule located in the intergluteal cleft, sometimes related to an ingrown hair.
- In women, it is less frequent than in men but can cause inflammation, pain, and risk of infection.
- Multiple origins: congenital or acquired (ingrown hairs), favored by a deep intergluteal fold, overweight, smoking, prolonged sitting position.
- Therapeutic solutions: emergency drainage in case of abscess, then surgical removal or laser treatment depending on the situation; long postoperative care.
- Prevention and follow-up: appropriate hygiene, hair management, smoking cessation, and attention to friction to reduce the risk of recurrence.
Pilonidal cyst in women: what it is and its origins
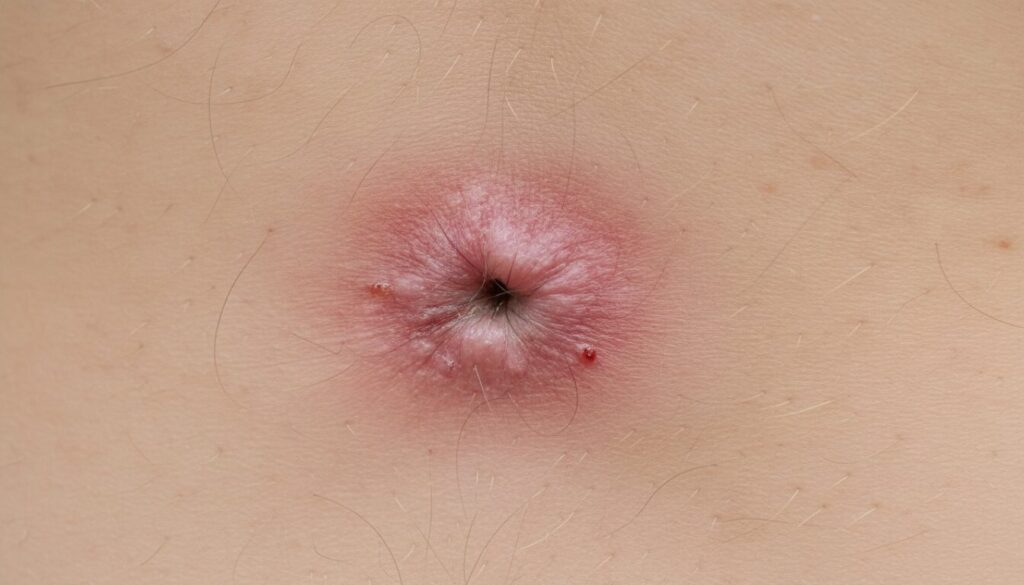
The pilonidal cyst, also called sacrococcygeal cyst or pilonidal sinus, is a benign lesion generally located in the hollow of the intergluteal cleft. It appears as a small nodule under the skin and can remain discreet as long as there is no inflammation or infection. In women, its frequency is lower than observed in men, but when it manifests it deserves appropriate attention to avoid complications and prolonged pain.
From a pathophysiological point of view, the formation of the pilonidal cyst is often explained by the entry of hairs into the epidermis. These hairs, sometimes thick or broken, penetrate the skin and are perceived as a foreign body by the body. An accumulation of sebum and a local inflammatory reaction then lead to the formation of a granuloma and a subcutaneous cavity: the cyst. This explanation, supported by clinical observations of dermatologist Erwin Benassaia, helps understand why hairiness and skin quality play a crucial role.
There are two main profiles of origin: the cyst can be congenital, present from childhood in a latent form, or acquired following an ingrown hair and repeated inflammation. Sometimes, the lesion remains silent for months before suddenly becoming superinfected, causing sharp pain and swelling. The average age of onset is between 15 and 40 years, making it a common pathology in young adults.
Let’s illustrate with a fictional clinical case serving as a thread: Sophie, 29 years old, office worker and young mother, notices a small bump in the hollow of the intergluteal cleft after several months of seated days and tight clothing. Initially painless, this small mass eventually reddens and becomes sensitive after an inflammatory flare-up. This scenario is common and highlights combined origins: prolonged sitting position, friction, and local hairiness. The analysis of this type of situation helps distinguish possible causes and guide diagnosis.
Clinically, understanding the cyst’s origin also helps anticipate preventive actions. If the origin is mainly related to an ingrown hair, targeted hair removal measures and local hygiene can reduce the risk of recurrence. Conversely, when the presented etiology is rather congenital, surveillance and specialized management are often necessary to avoid repeated infections. Final insight: identifying the origin — congenital or linked to a hair — directly guides the therapeutic and preventive strategy.
Symptoms of pilonidal cyst in women: recognizing inflammation and pain
Early recognition of symptoms allows action before inflammation worsens. The most frequent sign is a firm nodule palpable at the level of the intergluteal cleft. As long as the cyst is not superinfected, it can remain discreet and painless, but any change — redness, local heat, increased volume — should alert. In case of superinfection, the pain often becomes intense, constant, and sometimes pulsatile.
Suppuration leads to abscess formation, with painful swelling, redness, and sometimes purulent discharge. In some cases, mild fever may accompany the infection. Discomfort when sitting or during activities such as horseback riding is frequent, and the pain can disturb sleep and daily life. For young mothers, this discomfort can complicate care actions and increase stress related to family responsibilities.
Here is a practical list of signs to watch for:
- Presence of a nodule in the hollow of the intergluteal cleft, palpable under the skin.
- Redness and local heat indicating inflammation.
- Pain recurring or pulsatile, especially if the lesion is infected.
- Purulent or filamentous discharge when the sinus opens.
- Discomfort when sitting and during certain physical activities.
A concrete example: Marine, 34 years old, notices progressive pain over several days without fever. After two days of worsening, a discharge appears; consultation with a doctor allows rapid diagnosis of a pilonidal abscess and emergency drainage is performed. This case illustrates that progressive pain associated with discharge requires rapid management to limit the spread of infection.
Practically speaking, palpation and visual observation are essential. A doctor can make the diagnosis during a simple clinical examination, without systematic imaging, except in cases of suspected deep sinus tract or recurrence. Self-medication is discouraged: the use of anti-inflammatories can mask worsening, and inappropriate local care can delay necessary surgical treatment. Final insight: early recognition of inflammation helps reduce the duration of pain and the risk of severe infection.
Causes and risk factors: why some women develop a pilonidal cyst
Understanding the factors favoring a pilonidal cyst helps better target preventive actions. The formation of such a cyst is often multifactorial. Among the most frequently mentioned factors are a deep intergluteal fold, significant hairiness, oily skin, obesity, smoking, and prolonged sitting positions. Repeated friction and a lack of local hygiene can also contribute to hair penetration and the subsequent inflammatory reaction.
Mechanically, a deep intergluteal cleft creates a space where broken hairs can accumulate and rub against the skin. Sebum accumulation promotes drying and then hair breakage, facilitating their entry into the epidermis. Hairiness, naturally or after regrowth post-hair removal, increases the risk of anarchic regrowth and ingrowth. Moreover, smoking alters skin microcirculation and delays healing, which increases the probability of recurrence after treatment.
Here is a summary table comparing the main risk factors and their mechanisms:
| Risk factor | Mechanism | Clinical implication |
|---|---|---|
| Deep intergluteal fold | Promotes accumulation and friction of hairs | Increases the probability of hair entering the skin |
| Significant hairiness | More hairs likely to become ingrown | Risk of cyst formation and recurrence |
| Overweight | Increased pressure and friction | Discomfort and risk of inflammation |
| Smoking | Reduced microcirculation, impaired healing | Risk of postoperative complications and recurrence |
| Prolonged sitting position | Local compression and maceration | Promotes inflammation and superinfection |
In practice, the combination of several of these factors significantly increases the probability of cyst occurrence. Take the example of the thread: Sophie works long hours sitting, sometimes wears tight clothing, and has moderate hairiness. This combination creates a favorable environment for the formation of a pilonidal cyst. Conversely, an active woman with good local hygiene and hair management will have reduced risk.
Recent clinical studies confirm the predominance in the 15–40 age group and highlight the importance of lifestyle. In 2026, recommendations remain focused on reducing modifiable factors: smoking cessation, weight loss if needed, attention to hair removal methods rather than aggressive shaving which can promote ingrown hairs. Final insight: acting on modifiable risk factors is key to decreasing incidence and limiting recurrences.
Therapeutic solutions: surgical treatments, laser and alternatives
The choice of a therapeutic solution depends on the lesion’s state: uninfected cyst, acute abscess, or recurrent sinus. In case of a painful and suppurated abscess, emergency drainage to evacuate pus and relieve pain is required. This procedure prevents the spread of infection and prepares definitive management. Outside of an inflammatory flare-up, two main options are frequently offered: traditional surgical removal and laser treatment.
Classic surgery consists of excising the cyst under general anesthesia, often as outpatient care. Two approaches coexist: primary closure or leaving the wound open. The open technique, used to reduce the risk of recurrence, involves prolonged local care follow-up — sometimes up to two months — and may be perceived as disabling short term due to frequent dressings. Despite the duration of care, this method offers a lower probability of recurrence in many cases.
The laser technique (or less invasive method) is generally performed under local anesthesia in outpatient hospitalization. It allows ablation of the inflammatory tract with shorter sequences in terms of pain and recovery. However, the risk of recurrence is often slightly higher than that of a well-conducted excision. Dermatologist Erwin Benassaia emphasizes that the choice must be personalized according to the patient’s history, the extent of the sinus, and personal constraints.
It is important to note that removal is strongly recommended to avoid evolution towards recurrent abscess. Smoking cessation is essential to envision complete healing and limit recurrences, as smoking hinders healing. Furthermore, no exclusively medicinal approach replaces removal when the sinus is established and recurrent. Self-medication is discouraged and may delay appropriate intervention.
Precautions and practical steps before and after the therapeutic procedure:
- Medical consultation for diagnosis confirmation and treatment choice.
- In case of abscess: emergency drainage, then rescheduling of excision.
- Preoperative preparation: recommended smoking cessation, enhanced local hygiene.
- Postoperative care: regular dressings, healing monitoring, medical follow-up.
- Preventive measures to avoid recurrence: hair management, limiting friction.
A concrete example: Mélanie, 31 years old, chose classic surgery after two abscess episodes. Postoperative care lasted six weeks, with frequent dressings and gradual resumption of activities. After eight months, no new cyst was observed. This case shows that the recovery period is sometimes long but can lead to lasting resolution if recommendations are followed. Final insight: management must be individualized, with clear information on postoperative care and the key role of preventive measures to limit recurrences.
Prevention, follow-up, and daily life: practical advice to limit recurrences and manage pain
Prevention is at the heart of pilonidal cyst management. Simple actions, integrable into routine, can reduce the risk of occurrence or recurrence. Among them are appropriate hygiene, hair management, reduction of friction, and attention to modifiable risk factors such as smoking and overweight. These tips are especially useful for active women or young parents juggling professional and family responsibilities.
Daily practice: during showering, gentle cleaning of the intergluteal cleft with a mild soap is sufficient. Avoid using irritating antiseptics that can dry the skin and promote hair breakage. Regarding hair removal, durable methods like electrolysis or waxing followed by regular maintenance are often preferable to shaving, which can promote ingrown hairs. In case of surgery, a dressing surveillance protocol and follow-up consultation are essential.
Quick practical tips to try at the next shower:
- Gently clean the intergluteal cleft without excessive rubbing.
- Avoid tight clothing and prefer breathable fabrics.
- Limit prolonged sitting periods or use an appropriate cushion.
- If hairiness is a factor: discuss a durable hair removal solution with the doctor.
For medical follow-up, an appointment after removal is recommended to verify healing and prevent complications. In case of persistent pain or discharge, consult promptly. Health professionals can offer appropriate dressings or refer to paramedical solutions to limit daily discomfort.
The platform La Vie de Bébé offers resources to support families from the first days; although the pilonidal cyst is not strictly related to new parenthood, the reassuring and practical approach of this media helps manage care organization and the stress associated with chronic or recurrent pathologies. Finally, to optimize prevention, smoking cessation, weight loss, and lifestyle adaptation remain effective levers.
Practical example: for Sophie, establishing a small care ritual after showering (delicately drying the area, checking for redness, avoiding tight clothing in the evening) allowed identifying the start of inflammation before complication. Final insight: simple and regular actions offer significant margin to prevent inflammation and limit the occurrence of an abscess.
How to know if a pilonidal cyst is infected?
An infected pilonidal cyst manifests by redness, local heat, increased pain, purulent discharge, and sometimes fever. In presence of these signs, consult quickly for drainage and adapted treatment.
Is it possible to avoid surgery?
If the cyst is not superinfected and remains asymptomatic, monitoring and preventive measures can be proposed. However, for a recurrent sinus or an abscess, removal by surgery or laser is generally recommended to avoid new infections.
What to do to relieve pain before consultation?
Simple analgesics (paracetamol) and warm compresses can provide temporary relief. Avoid inappropriate local self-medication and consult if pain increases or discharge appears.
Does smoking influence healing?
Yes. Smoking impairs healing and increases the risk of postoperative complications and recurrence. Smoking cessation is strongly advised before any intervention to improve the chances of complete healing.