In brief
- White tongue in babies is often a milk residue, but can also indicate thrush (oral candidiasis), a common fungal infection in infants.
- Differentiating milk residue from thrush is done by observation: thrush forms thick plaques that do not come off easily and can affect the tongue, cheeks, and gums.
- Favoring factors include antibiotic intake, an immature immune system, reflux, or mother-baby transmission via the nipple.
- Diagnosis is clinically made by a professional; treatment is often local (antifungal in dropper or cream form) and rigorous hygiene is essential for prevention.
- Immediate actions to try: clean and sterilize pacifiers and bottles, wash hands and nipples before feeding, seek pediatric advice if there is pain, difficulty sucking, or persistent plaques.
Thrush in babies: how to recognize white tongue and its symptoms
When a child’s tongue changes from pink to white, many concerns arise. It is useful to know that a white tongue in infants is not always synonymous with illness. Often, it is simply milk residue after feeding. However, if this film persists and forms thick plaques, thrush, a fungal oral candidiasis caused by a fungus, should be considered.
To help parents decode the situation, here are concrete and observable elements. Milk residue usually appears immediately after feeding, is superficial, and dissipates with saliva or by very gently rubbing the tongue with a clean cloth. Thrush, on the other hand, manifests as thick whitish spots that adhere to the mucosa: tongue, inner cheeks, sometimes palate and gums.
What symptoms to watch for?
Several signs help to point to a probable thrush diagnosis:
- Persistent white plaques that do not come off easily with a clean finger or a damp cotton swab.
- Decreased appetite: the baby may suck less well or refuse the pacifier, a possible sign of oral discomfort.
- Irritability or crying during meals if there is pain.
- Bad breath sometimes noticeable, or digestive signs if the infection spreads.
Illustration by a concrete situation: Sophie, a young mother, notices that her son Mathis sometimes refuses the pacifier and has a tongue covered with plaques after several days. These spots do not go away when she rubs gently. The pediatrician suggests thrush and proposes a local treatment. This example shows the importance of observing the evolution over a few hours and consulting if discomfort persists.
A simple gesture to try at home: after a meal, wait a moment to see if the spots fade with saliva. If they persist, use a clean moistened cotton swab to rub gently. If the plaques do not move, note the location (tongue, cheeks, gums) and contact the health professional. This helps with diagnosis.
Finally, keep in mind that most cases of thrush in infants remain mild and regress with appropriate treatment. However, persistent feeding symptoms (refusal to suck) or intense irritability justify a prompt consultation. This vigilance helps avoid digestive complications and ensures the child’s well-being.
Key sentence: Observe whether white plaques adhere to the mucosa or disappear with saliva; this is the first clue that points to thrush or simple milk residue.
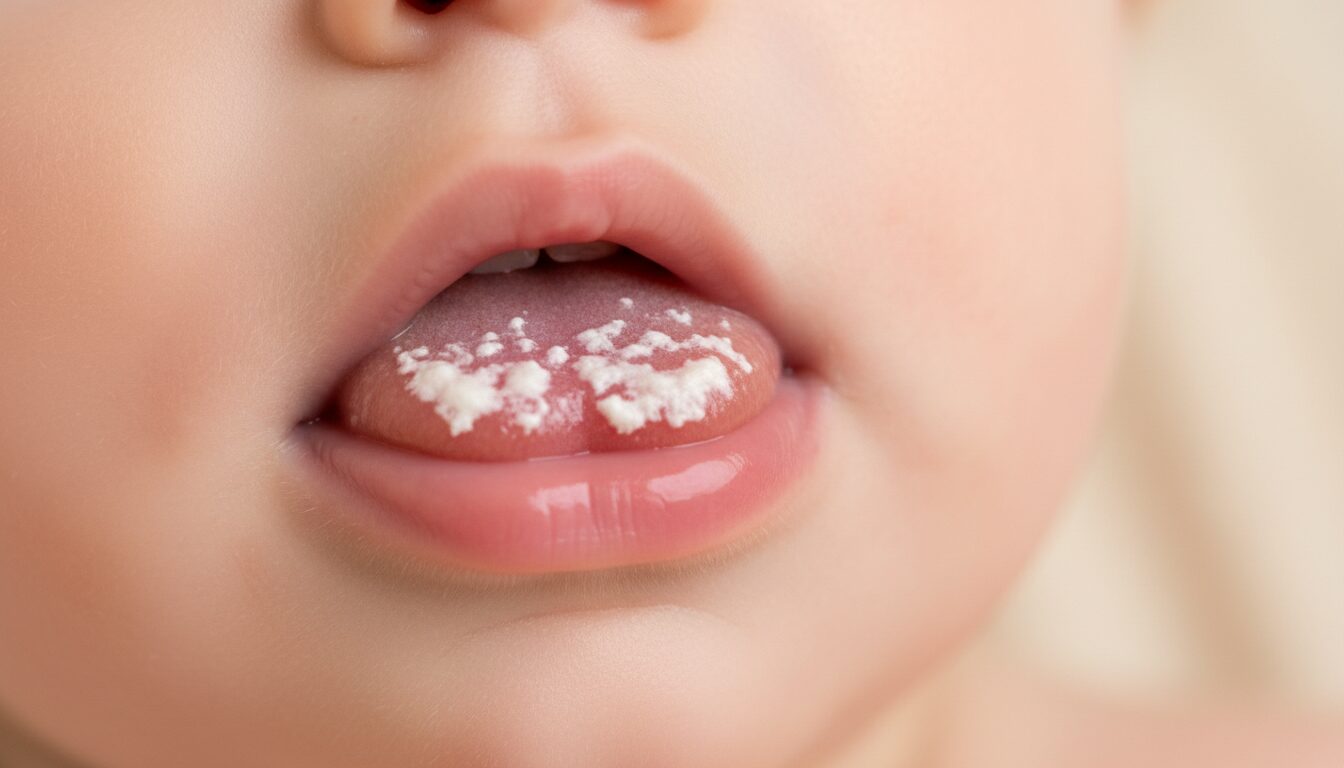
Origin of thrush in infants: understanding the fungal infection
Understanding the origin of thrush helps to accept the situation without guilt. The main culprit is Candida albicans, a yeast naturally present in the human body, notably in the digestive and vaginal flora. In healthy adults, it coexists without problem. In infants, the intestinal flora and immune response are still developing, which creates a fertile ground for yeast proliferation.
Several factors favor the appearance of oral candidiasis:
- Antibiotic therapy: antibiotics can disrupt the bacterial flora that naturally controls Candida, opening the way to fungal proliferation.
- Mother-baby transmission: yeast can pass from the nipple to the baby during breastfeeding if the mother has a nipple yeast infection, and vice versa.
- Gastroesophageal reflux disease (GERD): frequent reflux can favor deposits and local mucosal alteration.
- Low immunity: premature or fatigued infants are more vulnerable.
Concrete examples of infection initiation
Case A: a baby on antibiotics for an ear infection develops oral plaques a few days later. The doctor explains that the antibiotic altered the flora and that thrush is a known side effect.
Case B: a mother notes pain in her breast during feeding and observes white plaques on her nipple. The pediatrician examines the infant: there are also spots in the mouth. This is cross-transmission mother-baby, requiring treatment for both.
In 2026, clinical recommendations continue to emphasize the benign nature of thrush while reminding the importance of good hygiene and appropriate management in case of symptoms. Professionals stress prevention and mother-pediatrician coordination to treat both parties if necessary.
| Characteristic | Milk residue | Thrush (oral candidiasis) |
|---|---|---|
| Appearance | Light, diffuse film | Thick, well-defined white plaques |
| Location | Mainly tongue | Tongue, cheeks, palate, gums |
| Reaction to rubbing | Easily disappears | Does not remove completely |
| Associated symptoms | None or reflux | Decreased sucking, pain, irritability |
This table helps to quickly locate the origin of the problem. Methodical observation and knowledge of triggering factors facilitate early diagnosis. In case of doubt, a pediatric consultation remains the best response, especially if the mother observes signs on the nipple or if the child shows digestive symptoms.
Key sentence: Thrush often arises from an imbalance of flora and favoring factors (antibiotics, mother-baby transmission); understanding this allows action without guilt.
Practical diagnosis and guidelines for consultation
Diagnosis of thrush is mainly clinical: it is based on examining the mouth and observing symptoms. The doctor or midwife assesses the appearance of the plaques, their adherence, the impact on feeding, and any signs in the mother. No invasive examination is usually necessary for a healthy infant.
Concrete steps for diagnostic consultation
- Interview: date of onset, recent treatments (antibiotics), feeding (breast or bottle), possible digestive symptoms.
- Oral examination: observation of plaques on tongue, cheeks, palate, and gums; attempt to rub to check adherence.
- Feeding assessment: the pediatrician notes if the baby sucks less well or shows crying related to sucking.
- Therapeutic decision: prescription of a topical antifungal and hygiene advice; simultaneous treatment of the mother if necessary.
If the child shows signs of distress (persistent fever, total refusal to feed, signs of dehydration) or is premature or immunocompromised, additional examinations or stricter management may be considered. These situations remain rare but require increased responsiveness.
Before the consultation, several simple measures limit the spread: sterilize pacifiers and bottles, wash the nipple with soapy water before feeding if the mother is breastfeeding, and avoid sharing pacifiers or spoons. Giving probiotics on medical advice can help rebalance intestinal flora, especially if the child has received antibiotics.
A practical case: Lucas, 6 weeks old, had received antibiotic treatment for a neonatal infection. Three days after the end of treatment, the mother noticed a persistent white tongue. The pediatrician confirmed the diagnosis and prescribed a topical antifungal, with systematic cleaning of accessories. Recovery occurred in less than ten days. This example illustrates the importance of coordinated management.
To conclude this section, the key indicator is the persistence of plaques and the impact on feeding. These two elements direct toward quick consultation and appropriate treatment, preventing spread along the digestive tract.
Key sentence: Consult as soon as the white tongue persists and hinders sucking: spotting persistence and impact on feeding allows rapid diagnosis and effective treatment.
Treatments and practical care against oral candidiasis
Treatment of thrush aims to eliminate the yeast present in the mouth and, if necessary, in the entire digestive tract. In practice, the pediatrician often prescribes a local antifungal in the form of a solution to be applied inside the mouth (dropper) or a cream for the nipple if the child is breastfed. Sometimes, an additional oral treatment is recommended to eradicate digestive colonization.
Daily care and practical protocol
Here is a concrete, simple routine to implement:
- Apply the prescribed antifungal treatment at the hours recommended by the health professional.
- Clean after each feeding: sterilize pacifiers, bottles, teething rings, and any pacifier or toy put in the mouth.
- If the mother is breastfeeding, wash nipples and breasts with water and mild soap before each feeding; apply antifungal cream if prescribed.
- Maintain good hydration and monitor food intake: offer short and reassuring feedings if the baby shows discomfort.
- If on antibiotics, discuss with the pediatrician the possible addition of probiotics to support flora.
An example of application: the pediatrician prescribes an antifungal dropper to be administered after each feeding for 7 to 10 days. The mother sterilizes pacifiers and applies a cream on the nipple. After a week, the plaques decrease and feeding becomes comfortable again.
It is important to avoid self-medication. Antifungals are prescribed according to age and clinical state. The use of alcohol or homemade baking soda is not recommended without medical advice. Hygiene measures remain key: regular hand washing, sterilization, and simultaneous treatment of the mother if necessary.
Treatment of thrush generally allows a rapid return to feeding comfort. At the same time, reassuring parents plays a therapeutic role: knowing that the condition is common and treatable reduces anxiety and facilitates protocol adherence.
Key sentence: A local antifungal treatment combined with rigorous hygiene of objects and the nipple ensures rapid healing and reduces the risk of recurrence.
Daily prevention: simple actions to prevent thrush recurrence
Prevention is based on habits easy to integrate into daily life. The goal is to prevent the development of a favorable environment for Candida and avoid transmission between mother and baby. Here are practical and proven measures used in maternity and neonatology.
List of priority preventive actions
- Systematic hand washing before handling the baby or their equipment.
- Regular sterilization of pacifiers, soothers, bottles, and toys that go into the mouth.
- Breast hygiene: wash nipples with water and mild soap before feeding if symptoms appear.
- Avoid sharing pacifiers or utensils between babies or adults without sterilization.
- Medical follow-up during antibiotic therapy: discuss probiotic supplementation with the pediatrician.
A practical gesture for active families: organize a small “clean pacifier” kit in the diaper bag containing a closed case and sterile wipes for outings. This limits the temptation to give non-sterilized objects to the baby outside.
The platform La Vie de Bébé offers practical guides and educational sheets to easily integrate these actions, with routines adapted to the infant’s first weeks. Consulting a reliable resource helps feel supported without being overwhelmed by information.
For fragile families (premature, immunocompromised children), pediatricians recommend increased vigilance and sometimes reinforced measures. But for the majority of families, simple gestures suffice to limit recurrences.
Finally, the role of kind follow-up is crucial: note the onset of symptoms, openly discuss with the health professional, and follow prescriptions to prevent the chronic establishment of candidiasis. These small habits transform an anxiety-provoking situation into a soothing routine.
Key sentence and action to try: From the next diaper change, sterilize a pacifier and wash hands before feeding; it is a simple gesture that significantly reduces transmission risk and promotes the baby’s comfort.
How to differentiate milk residue from real thrush?
Milk residue disappears with saliva or gentle rubbing. Thrush forms thick white plaques that adhere and can affect tongue, cheeks, and gums. If the spots persist despite slight rubbing, consult a professional.
Should breastfeeding be stopped if the baby has thrush?
No, breastfeeding can generally continue. It is however recommended to wash nipples with water and soap before feeding and to follow pediatrician’s advice, who may prescribe an antifungal cream for the mother if necessary.
Which objects should be sterilized in case of thrush?
Sterilize pacifiers, bottles, teething rings, soothers, and toys put in the mouth. Also wash wipes and towels in contact with the baby’s mouth. This prevents recontamination.
Are probiotics useful to prevent thrush after antibiotics?
On medical advice, probiotics may help rebalance the intestinal flora after antibiotic treatment. Discussing with the pediatrician allows adapting the strain and dosage to the child.

