In brief :
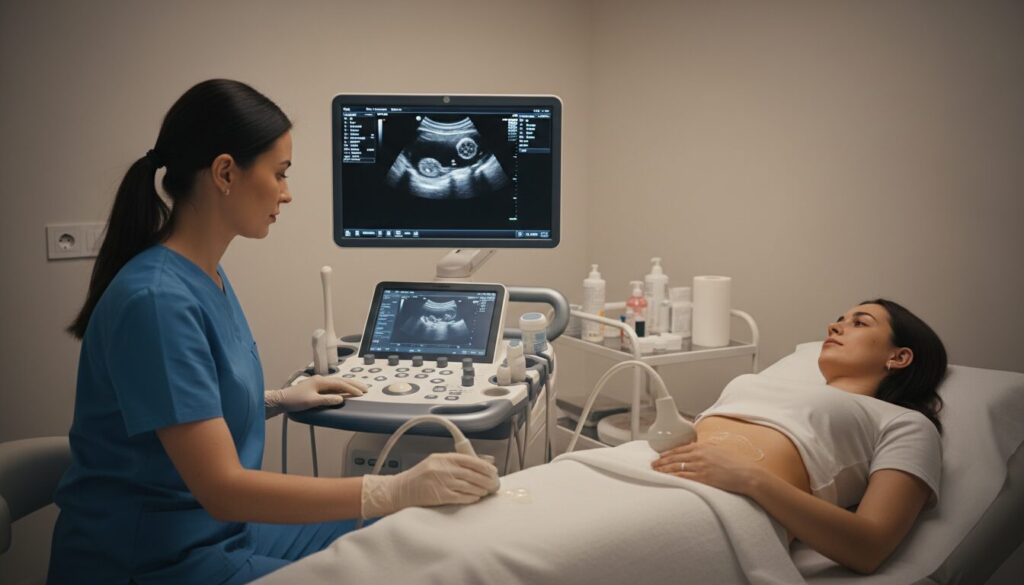
- Pelvic ultrasound includes abdominal ultrasound (suprapubic) and endovaginal ultrasound, two complementary techniques to visualize pelvic organs.
- The medical exam preparation is simple: hydration recommended, no cream or oil, report any latex allergy.
- The ultrasound procedure is explained step by step: interview, abdominal exam then possibly endovaginal, immediate results in most cases.
- The ultrasound technique is based on ultrasound waves, without irradiation, with real-time images for pelvic diagnosis and visualization of pelvic organs.
- Indicative cost: between €52 and €70, reimbursed at 70% by Social Security; the mutual insurance generally covers the remainder.
Pelvic ultrasound: why and when to prescribe an abdominal or endovaginal ultrasound
The decision to perform a pelvic ultrasound always relies on a precise clinical indication. This exam is not requested randomly: it aims to address symptoms or monitor a particular situation.
Common reasons include pelvic pain, abnormal bleeding, irregular menstrual cycles, suspicion of an ovarian cyst, fibroid, or endometriosis. The exam also takes place during pregnancy monitoring, for fetal location and growth surveillance, as well as in medically assisted procreation (MAP) pathways to monitor follicular maturation.
Main indications and benefits
For a patient like Amélie, worried due to irregular cycles and localized pain, the ultrasound helps differentiate a benign cause (functional cyst) from a pathology requiring follow-up or intervention. The exam can also confirm the correct position of an intrauterine device or assess uterine vascularization when needed.
In men, visualization of pelvic organs via pelvic ultrasound focuses on the bladder and prostate; in doubtful cases, an endorectal approach is sometimes used for increased precision.
When to choose abdominal or endovaginal approach?
Abdominal ultrasound (or suprapubic) involves placing a probe on the lower abdomen. It is simple and non-invasive and often constitutes the first step. If the images are not clear enough, or if the exam requires millimetric precision—such as for early pregnancy dating or MAP follow-up—endovaginal ultrasound is indicated.
Endovaginal ultrasound uses an elongated probe inserted into the vagina, covered with a sterile sheath, to get closer to the organs and improve image quality. This approach is particularly useful for viewing the cervix, uterus, and ovaries.
Illustrated clinical example
Amélie consults for subacute pelvic pain. The practitioner starts with an abdominal ultrasound; the images reveal a poorly defined ovarian mass. The exam is completed with an endovaginal ultrasound, which identifies a 4 cm functional cyst without alarming signs. The diagnosis avoids unnecessary surgery and allows simple follow-up. This sequence illustrates how the two techniques complement each other for a reliable pelvic diagnosis.
Insight: in the presence of a gynecological symptom, pelvic ultrasound often remains the key exam to guide management.
Preparation for abdominal or endovaginal ultrasound: practical advice
Preparation for a pelvic ultrasound is generally simple and not very restrictive, but some practical precautions ensure a quicker and more comfortable exam.
The main recommendation is to avoid applying creams or oils on the area to be examined, as these products can alter ultrasound transmission and reduce image quality.
Hydration and bladder: what to do?
Depending on the exam’s objective, the practitioner may ask to arrive with the bladder more or less full. In most current cases, sufficient hydration the day before and the day of the exam is enough. The important thing is that the patient is comfortable: an overfull bladder causes discomfort, while an empty bladder can make visualization more difficult for certain indications.
For exams targeting the bladder or screenings such as endometriosis, a full bladder may be requested to better locate certain organs. Always ask for specific instructions from the office secretary or medical team.
Allergies, menstruation, and consent
Reporting any allergy is important, especially to latex products. The probe covers are often made of latex: if an allergy is known, inform the practitioner in advance to arrange an appropriate cover.
The exam is not systematically contraindicated during menstruation; the decision takes into account the patient’s comfort and the reason for the ultrasound. Consent is obtained after a brief interview explaining the purpose and procedure.
Practical table: quick preparation
| Situation | Recommended preparation | Note |
|---|---|---|
| Early pregnancy monitoring (dating) | Hydration, sometimes full bladder | Endovaginal approach often used if very early |
| Pelvic pain / cyst | No cream, normal hydration | Start with abdominal approach, completed if necessary |
| Prostate screening (men) | Hydration as instructed | Suprapubic or endorectal approach depending on required precision |
| Latex allergy | Report before appointment | Alternative protection provided |
Insight: simple preparation and clear communication with the team reduce stress and improve exam quality.
Ultrasound procedure: step by step for a reassuring abdominal or endovaginal ultrasound
The ultrasound procedure follows a clear logic: interview, positioning, abdominal exam, then endovaginal supplements if necessary. The duration generally varies between 15 and 30 minutes depending on complexity.
Upon arrival, a brief exchange explains the reason for the exam and reassures the patient about each stage. The room is often dimmed to facilitate image viewing.
The first step: abdominal ultrasound
The patient lies on her back, knees bent. The practitioner applies an aqueous gel, sometimes cold, which improves contact between the probe and the skin. The probe is moved over the lower abdomen to explore the uterus, ovaries, and bladder.
This approach is non-invasive and already provides much information, notably the presence of a mass, organ size, or position of an intrauterine device.
If necessary: complete with an endovaginal ultrasound
If abdominal ultrasound does not offer sufficient precision, the endovaginal probe is proposed. It is covered with a sterile sheath and lubricated with a water-based gel.
The probe is inserted gently; the patient may prefer to insert it herself if this gives a feeling of control. The exam is not painful but can be uncomfortable; the practitioner adapts the technique to the patient’s sensitivity and stops if discomfort becomes too intense.
Communication and results
Many practitioners describe aloud what they observe, allowing real-time tracking of the exam. Images are analyzed on screen and several measurements are taken. In most cases, a verbal report is given immediately, followed by a written report transmitted to the prescribing doctor.
For Amélie, transparency throughout the ultrasound procedure turned an anxiety-inducing experience into an informative consultation: clear explanation, possibility of self-insertion of the probe, and rapid report delivery.
Insight: the quality of listening and explanation during the exam contributes as much to comfort as the quality of the images obtained.
Ultrasound technique, interpretation and follow-up: how to read pelvic medical imaging
The ultrasound technique uses high-frequency sound waves. They bounce off tissues and create images based on the density and composition of organs. Unlike X-rays, there is no exposure to ionizing radiation.
Image reading requires expertise: measuring the size of a cyst, assessing the vascularization of a fibroid, or monitoring the evolution of an embryo requires precise landmarks. The trained practitioner, such as a midwife sonographer or radiologist, integrates these elements to establish a reliable pelvic diagnosis.
Examples of common interpretation
A simple ovarian cyst appears as a black (fluid) formation without thick walls or vascularization. A uterine fibroid appears as a solid mass with clear contours. Endometriosis may require special slices and an extended assessment for proper evaluation.
Doppler can complement the exam to assess vascularization, useful for distinguishing some benign masses from suspicious lesions.
Cost, reimbursement and practical advice after the exam
A pelvic ultrasound usually costs between €52 and €70 depending on the clinic. It is covered at 70% by Social Security; the remainder is usually covered by the mutual insurance according to the contract. In case of extra fees, the mutual insurance reimburses according to the coverage.
After the exam, follow-up is generally simple: no side effects related to ultrasound. If an invasive procedure is planned, the practitioner will explain options and organize follow-up. The timing of management depends on the diagnosis and clinical urgency.
For more practical articles and human support about parenthood and gynecological health, the platform La Vie de Bébé offers validated resources and concrete advice.
Insight: pelvic medical imaging provides quick and reliable answers when the exam is entrusted to a trained practitioner and indications are clear.
Practical advice, precautions and FAQ to approach a pelvic ultrasound calmly
Approaching a pelvic ultrasound with concrete reference points helps reduce stress and achieve an effective exam. Here are tips drawn from clinical experience and oriented towards patient comfort.
Communication is central: ask the practitioner what they will look at, request breaks if discomfort increases, and report any allergy or discomfort. Respect for privacy and consent are explicit rights.
Checklist before leaving for the appointment
- Check the instruction concerning the bladder (full or not).
- Do not apply cream, oil, or product on the abdomen.
- Report any latex allergy or particular sensitivity.
- Bring the medical prescription and monitoring book if pregnant.
- Wear comfortable clothing to facilitate positioning.
These simple gestures facilitate the team’s work and improve diagnostic quality.
Specific precautions
Endovaginal ultrasound is contraindicated in young women who have not had sexual intercourse involving penetration, except for very precise medical indication and after discussion. In case of significant pain during the exam, stopping is systematically proposed.
Finally, managing expectations is essential: ultrasound often excludes immediate fears, but it does not eliminate the need for follow-up if a diameter, mass, or suspicious sign is observed.
Insight: preparing for the exam and knowing what questions to ask transforms a potentially anxiety-provoking consultation into a useful and reassuring moment.
Is pelvic ultrasound painful?
No, pelvic ultrasound is normally not painful. It can be uncomfortable, especially endovaginal ultrasound, but the practitioner adapts their technique and the exam can be stopped if pain is significant.
Should I come with a full bladder?
It depends on the indication. In most cases, good hydration is enough, but for some assessments (bladder, endometriosis), a full bladder may be requested. Follow the instructions given when making the appointment.
What is the price of a pelvic ultrasound and its reimbursement?
The price usually ranges between €52 and €70. Social Security reimburses 70% and the rest is partially covered by the mutual insurance depending on the contract. In case of extra fees, coverage depends on the mutual insurance.
Why choose endovaginal ultrasound rather than abdominal?
Endovaginal ultrasound offers better resolution to visualize the cervix, uterus, and ovaries, because the probe is closer to the organs. It is chosen when millimetric precision is necessary or if abdominal ultrasound is insufficient.